Author Information1
Endlaw, S.2; Farhan, H.3.; Li, J.4; Peng, C.5; Skaggs, S.3; Tan, A.6
(Editor: Koizumi, N.7)
1 All authors are listed in alphabetical order.
2 Chantilly High School, VA, 3George C. Marshall High School, VA, 4Thomas S. Wootton High School, CA, 5Tesoro High School, CA, 6San Mateo High School, CA,
7George Mason University, VA
Background: Systemic lupus erythematosus (SLE) is an autoimmune disease with both high morbidity and mortality rates [1]. Clinical symptoms, laboratory findings, and optional biopsy results are the basis for early diagnosis of SLE. The disease is well-known for its butterfly rash that appears mainly on women at child bearing ages, and patients should be treated with antimalarials with hydroxychloroquine presenting the best results; it has a higher rate of remission, fewer relapses and reduced damage in the course of the disease [2]. Although there has been significant progress made in regards to SLE, the number of SLE patients who face End Stage Renal Disease (ESRD) has increased from 1.6 to 4.9 million from 1982 to 2004 [3]. Patients with ESRD were tested to predict a 3-year allograft survival after transplantation. Graft has an 84% chance of 3-year survival if the patient didn’t need dialysis during the first week compared to 58% if dialysis was needed during the first post transplantation week. For those who had needed dialysis for the first week, if their maintenance immunosuppressive regimen contained prednisone, took hemodialysis, and was older than 50 years, their graft had a lower probability of survival [1]. Adding on, much advancement and findings regarding SLE has led to the discovery of correlation between the disease and minority populations. The Centers for Disease Control and Prevention National Lupus Registries found that people of color (African Americans, APIs, and Hispanics) are more susceptible to SLE. Studies show that psychosocial stressors are potential exacerbators of SLE which can activate the inflammatory pathways. Often exposed to racial discrimination, people of color experience a large source of stress which can cause many health disparities, which in turn, can lead to the further worsening of SLE [4]. It has also been studied that after a kidney transplant, many patients have gotten rid of their Lupus while others, specifically African Americans (AA) have gotten Lupus back with other symptoms [3]. Adding on, five years after a kidney transplant for Lupus Nephritis (LN) graft survival for AF is at 63%, while for non-AA the graft survival rate is at 78.3%. Further, AA of lower median household income (MHI) are more likely to experience quicker graft loss compared to AA of higher MHI. For non-AA, there was no significant trend between MHI and graft loss [5]. While LN significantly increased the risk of graft failure, rejection remained the primary driver of graft failure incidence. These results emphasized that these findings should not discourage patients with Lupus from considering a kidney transplant [6].
Objective: The study investigated how the outcomes of kidney transplants differ by sex and race in the transplant recipients with SLE diagnosis.
Methods: A retrospective analysis was performed using the UNOS database between January 1, 2010 and June 30, 2022. The basic patient, donor and transplant characteristics were compared by recipient sex and ethnicity using T- and Chi-sq. tests. Survival curves and the estimates for transplant outcomes by sex and ethnicity were obtained using the Kaplan-Meier (KM) Product Limit method. In the analysis, patient death and graft failure were the end-points. Patients who did not experience any of the end-points or whose life and graft status was unknown were censored on the last follow-up or the last day of the study. Log-rank tests were used to test the equality of the curves. All analyses were done in R and the statistical significance was defined by p<0.05.
Results: Overall, male patients were more likely to experience the graft failure. African American patients were also more likely to experience the graft failure (p<0.001) while Asians and Hispanic patients were less likely to experience the graft failure (p<0.001).
Table 1. Descriptive Statistics
| Patient Sex and Ethnicity | No Graft Failure (n = 3300) | Graft Failure (n = 837) | p-value |
| Male, n (%) | 552 (16.73%) | 172 (20.55%) | 0.011 |
| White | 559 (16.94%) | 166 (19.83%) | 0.554 |
| African American | 1614 (48.91%) | 474 (56.63%) | < 0.001 |
| Hispanic | 785 (23.79%) | 143 (17.08%) | < 0.001 |
| Asian | 276 (8.36%) | 41 (4.10%) | < 0.001 |
| Other | 66 (2%) | 13 (1.55%) | 0.483 |
Figure 1. Kaplan Meier Survival Curves for Graft Failure
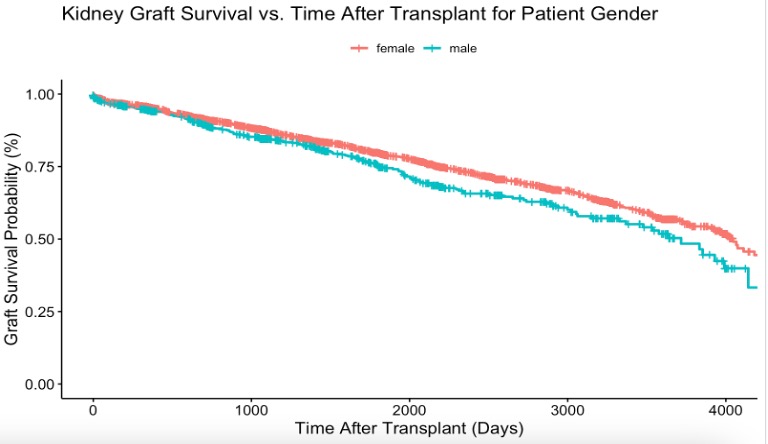
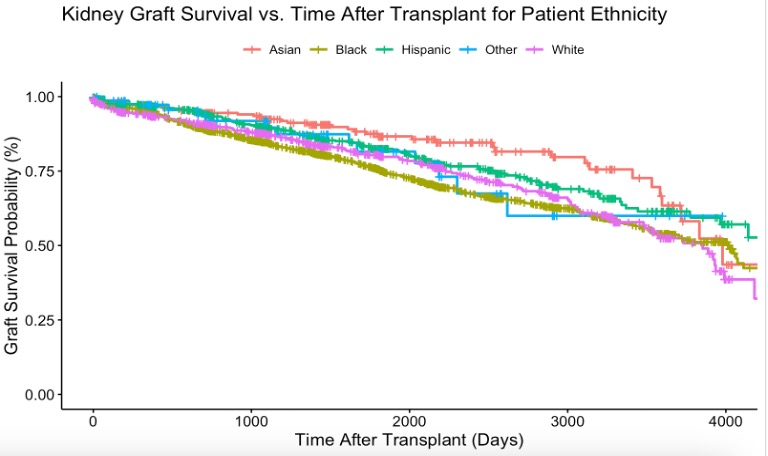
Conclusions: Male and African American patients are at higher risk for graft failure among the kidney transplant recipients whose primary diagnosis was SLE.
References
- Tang, H., Poynton, M.R., Hurdle, J.F., Baird, B.C., Koford, J.K. and Goldfarb-Rumyantzev, A.S., 2011. Predicting three-year kidney graft survival in recipients with systemic lupus erythematosus. Asaio Journal, 57(4), pp.300-309. doi: 10.1097/MAT.0b013e318222db30
- Kuhn, A., Bonsmann, G., Anders, H.J., Herzer, P., Tenbrock, K. and Schneider, M., 2015. The diagnosis and treatment of systemic lupus erythematosus. Deutsches Ärzteblatt International, 112(25), p.423. doi: 10.3238/arztebl.2015.0423
- Lionaki, S., Skalioti, C. and Boletis, J.N., 2014. Kidney transplantation in patients with systemic lupus erythematosus. World Journal of Transplantation, 4(3), p.176. doi:10.5500/wjt.v4.i3.176
- Drenkard, C. and Lim, S.S., 2019. Update on lupus epidemiology: advancing health disparities research through the study of minority populations. Current opinion in rheumatology, 31(6), p.689. doi:10.1097/BOR.0000000000000646
- Nee, R., Jindal, R.M., Little, D., Ramsey-Goldman, R., Agodoa, L., Hurst, F.P. and Abbott, K.C., 2013. Racial differences and income disparities are associated with poor outcomes in kidney transplant recipients with lupus nephritis. Transplantation, 95(12), pp.1471-1478. doi:10.1097/TP.0b013e318292520e
- Contreras, G., Mattiazzi, A., Guerra, G., Ortega, L.M., Tozman, E.C., Li, H., Tamariz, L., Carvalho, C., Kupin, W., Ladino, M. and LeClercq, B., 2010. Recurrence of lupus nephritis after kidney transplantation. Journal of the American Society of Nephrology: JASN, 21(7), p.1200. www.ncbi.nlm.nih.gov/pmc/articles/PMC3152228/.
